The IRS increased tax deductible limits for traditional long-term care insurance premiums paid in 2017. Jesse Slome, director of the American Association for Long-Term Care Insurance (AALTCI) said, “The tax deductibility of premiums…provides a real incentive for consumers, especially after retirement.” Only traditional long-term care insurance policies may be tax-deductible to an individual. Special tax advantages are not available for linked-benefit products, such as life insurance or annuity policies that provide a long-term care benefit. According to the AALTCI, in 2016 more people will purchase combo products than those who purchase traditional LTC insurance policies. IRS reports for 2014 reveal that nearly 5.1 million tax filers with incomes of $40,000 to $100,000 reported medical expenses that exceeded adjusted-gross income limits. Starting in 2017, all individuals can deduct qualified medical expenses that exceed 10% of adjusted gross income for the year. The limit is 7.5% of adjusted gross income for 2016, for individuals 65 and older. The IRS allows individuals to deduct medical expenses including preventative care, dental and vision care, prescription medications, glasses, contacts and hearing aids. Traditional long-term care insurance premiums can be included in the term “medical care.” “For retired seniors,…reduced income and increased medical costs means that the cost of traditional long-term care insurance can be all or mostly tax deductible. Many seniors have medical expenses that don’t meet the adjusted gross income limit. But they exceed the limit when the cost of long-term care insurance is included, which provides a significant tax deduction. This is a real benefit for the 23 million individuals age 65 or older who file federal tax returns,” said Slome. The following are the just announced 2017 limits:
The IRS increased tax deductible limits for traditional long-term care insurance premiums paid in 2017. Jesse Slome, director of the American Association for Long-Term Care Insurance (AALTCI) said, “The tax deductibility of premiums…provides a real incentive for consumers, especially after retirement.” Only traditional long-term care insurance policies may be tax-deductible to an individual. Special tax advantages are not available for linked-benefit products, such as life insurance or annuity policies that provide a long-term care benefit. According to the AALTCI, in 2016 more people will purchase combo products than those who purchase traditional LTC insurance policies. IRS reports for 2014 reveal that nearly 5.1 million tax filers with incomes of $40,000 to $100,000 reported medical expenses that exceeded adjusted-gross income limits. Starting in 2017, all individuals can deduct qualified medical expenses that exceed 10% of adjusted gross income for the year. The limit is 7.5% of adjusted gross income for 2016, for individuals 65 and older. The IRS allows individuals to deduct medical expenses including preventative care, dental and vision care, prescription medications, glasses, contacts and hearing aids. Traditional long-term care insurance premiums can be included in the term “medical care.” “For retired seniors,…reduced income and increased medical costs means that the cost of traditional long-term care insurance can be all or mostly tax deductible. Many seniors have medical expenses that don’t meet the adjusted gross income limit. But they exceed the limit when the cost of long-term care insurance is included, which provides a significant tax deduction. This is a real benefit for the 23 million individuals age 65 or older who file federal tax returns,” said Slome. The following are the just announced 2017 limits:
Attained Age
Before Close of
Taxable Year 2017 Limit 2016 Limit
–––––––––––––––––––––––––––––––––––––––––––––––––––
40 or younger $410 (+ 5.1%) $390
40+ to 50 $770 $730
50+ to 60 $1,530 $1,460
60+ to 70 $4,090 $3,900
70+ $5,110 (+4.9) $4,870
Source: IRS Revenue Procedure 2016-55 (2017 limits) and 2015-53 (2016 limits)
For more information, visit www.aaltci.org or call the organization at 818-597-3227.
How the Medicare Enrollment Maze Puts Seniors at Risk
Transitioning to Medicare is a big problem for seniors, according to a study by the American Institutes for Research. Researchers surveyed 17 health insurance counselors, brokers, insurers, large employers and consumer advocates who work with seniors. Since 2000, the age to collect full Social Security retirement benefits has risen from 65 to 67, and people are working longer, slowly fraying the decades-old enrollment link between Social Security and Medicare and confusing millions of older Americans, according to the study. “Seniors who take a wrong turn through the Medicare enrollment maze can face coverage gaps, disrupted care, large out-of-pocket costs, and lifelong late-enrollment penalties,” said Kathryn Paez, a principal researcher at AIR and lead author of the study.
Suppose that a person turns 65, and they or a spouse keeps working and maintains employer health coverage instead of retiring and enrolling in Social Security. They must sign up for Medicare, especially Part B, which covers physician and other outpatient care. Otherwise, they risk coverage gaps and expensive lifelong Part B late-enrollment penalties. People who delay Social Security retirement benefits until after 65 get no official government notice about how to avoid penalties or gaps in coverage, Paez said.
This problem is likely to worsen as the full Social Security retirement age reaches 67 for those born in 1960 or later and more Americans work past 65. Since 2000, the proportion of Americans enrolling by age 65 has dropped by 20% to 61.5% in 2014. Avoiding penalties when people continue to work past age 65 depends largely on whether their employer coverage is primary or secondary to Medicare. That depends on whether coverage is based on employment and the number of people employed by employer. In some cases, an individual must enroll in Medicare during a special enrollment period or face lifelong Part B late-enrollment penalties and go up to 16 months without coverage.
All Part B enrollment periods have different time frames for applying and schedules for when coverage takes effect. To confuse matters more, all Part B enrollment periods differ from the annual open enrollment period each fall when people can change their Medicare Part D, Medigap or Medicare Advantage coverage.
People who miss the Part B enrollment window pay a lifetime late-enrollment penalty equal to 10% of the standard Part B premium for each full 12-month period they could have had Part B had they enrolled. The penalties can add up over a lifetime. For example, a woman who pays a 30% late fee would pay $9,769 extra for Part B coverage; men, whose life expectancy is shorter, can expect to pay $8,641.
Even with extensive online and print resources, many beneficiaries need personalized counseling to make informed choices. The SHIP state-run programs get federal grants train and manage a network of staff and volunteer Medicare counselors who provide free counseling to beneficiaries. Medicare beneficiaries are inundated with mail and ads about Medicare plans when they turn 65 and during the annual fall open enrollment period. Feeling overwhelmed and unsure of where to start, some beneficiaries seek out a SHIP or broker. Others may want a second opinion after doing their own research.
SHIP appears to offer a highly cost effective way to provide one-on-one support to help Medicare beneficiaries make more informed choices about their coverage. In 2013, the $52 million spent on SHIP provided one-on-one counseling to more than 2.6 million of the 52.5 million Medicare beneficiaries at a cost of less than $20 per beneficiary served.
Possible policy solutions include requiring the federal government to notify all people approaching age 65 of Medicare enrollment requirements, educating employers about transitioning older workers to Medicare coverage, streamlining and harmonizing Medicare enrollment periods, enhancing health insurance counseling services for older Americans, and strengthening appeal rights for beneficiaries facing late-enrollment penalties. For more information, visit www.air.org.
Medicaid Pharmacy Could Save Billions
Medicaid could save $51.1 billion over the next 10 years while maintaining or improving the quality of care. They key is implementing the full range of pharmacy benefit management (PBM) tools, according to a report by the Menges Group. The following is a breakdown of ways to save money over 10 years:
- Save $26.5 billion by optimizing the use of generic drugs: Generics are not always the lowest net cost products for state Medicaid programs. Each percentage point increase in the generic dispensing rate reduces prescription drug costs by 3%
- Save $2.4 billion by encouraging more affordable, preferred brands: State Medicaid programs that exempt entire drug classes from preferred drug list reviews make it harder to use prior authorization protocols that encourage safe and cost-effective drug utilization.
- Save $1.9 billion in reduced drug diversion, polypharmacy, fraud, and waste: Medicaid plans that are more actively managed detect patterns of fraud with tools like step therapy, audits, and pharmacy lock-in programs to help detect and avoid inappropriate utilization.
- Save $11.4 billion by negotiating better discounts from drugstores that want to participate in more selective pharmacy networks: State Medicaid programs could save by implementing competitive pharmacy contracting processes that characterize Medicare Part D and commercial-sector programs. In Medicare Part D, preferred pharmacy options have demonstrated savings of 6.1%.
- Save $9 billion by aligning pharmacy reimbursements with competitive levels in the commercial sector: CMS has recently required states to adopt an Actual Acquisition Cost (AAC) methodology for paying pharmacies. The AAC approach may result in higher pharmacy reimbursements than the already higher-than-average reimbursements characteristic of traditional Medicaid programs.
For more information, visit www.pcmanet.org.
Enrollment in Consumer-Directed Health Plans Jumps Nearly 22%
Consumer-directed health plans (CDHPs) have increased in prevalence in all regions except the West, which saw the number of plans decrease by 7.2% from 2015. However, in the West, there was an 18.9% increase in the number of employees enrolled, indicating the continued attraction to their lower premiums, according to a survey from United Benefit Advisors (UBA). While most of the country is experiencing slightly increased premiums, California has enjoyed an 11.4% decrease in average single premiums. California Employers are moving away from CDHPs and toward HMOs, which the survey shows are 9% less costly than the average plan.
Twenty-six percent of U.S. employees are enrolled in CDHP plans, an increase of 22% from last year and nearly 70% from five years ago. CDHP plan costs have risen 2% from last year. So while they are still 3.5% less costly than the average plan, they offered more savings in 2015 when they were 5.6% less than the average plan. “CDHP interest among employers isn’t surprising given these plans’ savings over the average plan. Employees typically pick up 32% of the cost, slightly below the 35% average employee contribution rate among all plans, making them an attractive choice for many employees as well. But like all cost benchmarks, plan design plays a major part in understanding value,” said Les McPhearson, CEO of UBA. Twenty-six percent of plans offered by employers are CDHPs, a 14.2% increase in the past five years. Regionally, there are major differences in CDHP popularity. CDHPs account for the following percentage of plans offered by employers:
- Northeast 34%
- North Central 33%
- Southeast 26.6%
- Central 21%
- West 14%
McPhearson said, “Cost-saving strategies, like cost shifting, should be taken with a grain of salt, given the increased burdens they place on employees, Given the higher than average out-of-pocket costs of CDHPs, this turbulence in the West, which typically leads the nation in health care trends, indicates that employers and employees are still determining the value and success of these plans, making it a cautious upward trend to watch.” For more information, visit www.UBAbenefits.com.
An Update on HSA Balances and Contributions
Based on an analysis of 2014, The Employee Benefit Research Institute (EBRI) offers these facts about HSA-eligible health plans:
- Starting from nothing about a decade ago, enrollment in HSA-eligible health plans was about 17 million policyholders and their dependents in 2014.
- The average HSA balance at the end of 2014 was $1,933, up from $1,408 at the beginning of the year.
- Average account balances increased with the age of the account owner. Account balances averaged $655 for owners under 25 and $5,016 for owners 65 and older.
- About 6% of HSAs had an associated investment account. End-of-year 2014 balances were higher in accounts with investment assets. Thirty-seven percent of HSAs with investment assets ended 2014 with a balance of $10,000 or more compared to 4% of HSAs without investment assets.
- Among HSAs with investment assets, accounts opened in 2014 ended the year with an average balance of $6,544; whereas those opened in 2005 had an average balance of $19,269 at the end of 2014. HSAs with individual or employer contributions accounted for 70% of all accounts and 86% of the assets in 2014. Four percent of these accounts ended the year with a zero balance
- On a yearly average, individuals who made contributions deposited $2,096 to their account. HSAs receiving employer contributions got an average of $1,021 a year.
- Four-fifths of HSAs with a contribution also had a distribution for a health care claim during 2014. The average amount distributed for health care claims was $1,951.
- Distributions for health care claims increased with age, except among those 65 and older. Average annual distributions were $636 for account owners under 25, $2,373 for account owners 55 to 64, and $2,124 for account owners 65 and older. However, the likelihood of taking a distribution for health care claims was higher among accounts opened more recently. For more information, visit ebri.org.
New FDA Regulation Allows Dermatologists To Customize Patient Prescriptions
Prescriber’s Choice, a Florida-based pharmaceutical company, has created a new model for dermatological prescriptions in which medications can be customized and dispensed during the office visit. Soaring prescription drug costs have generated outrage among physicians and patients. Some drugs- even generics-carry eye-popping costs and health plans are increasingly asking people to shoulder more of the cost, according to a recent American Academy of Dermatology article. People often leave the pharmacy without their prescribed medication. Dr. Spencer Malkin, the CEO of Prescriber’s Choice is working with doctors to create customized prescriptions for patients to be dispensed at the time of the office visit. Dr. Malkin said, “Instead of patients presenting to a pharmacy, dealing with medication substitutions, and being floored by the out-of-pocket expenses, they get a customized medication directly from their physician at the time of their appointment. In addition, it has the potential to save the healthcare system billions, as there is nothing being billed to the insurance carriers. The physicians are able to practice unencumbered by third-party payors; patients get medications that are tailored to their conditions; and there are substantial cost savings to the patient and to the health system. This restores balance to a specialty that has experienced a shift away from the medical practice of dermatology and toward cosmetics and aesthetics.” For additional information, visit www.prescriberschoice.com.
DMHC Seeks Innovators
The Dept. of Managed Healthcare extended it deadline for the state’s Let’s Get Healthy California Innovation Challenge to Monday, October 31. The following are some entries:
- Vivity is an Anthem Blue Cross health benefit plan that brings together multiple hospital systems to create a virtually integrated delivery system. There is a joint risk-sharing arrangement for institutional services among Anthem Blue Cross and seven participating hospital systems.
- Light Bridge Medical Associates & Health Net offer a program is designed to mine health system data to identify patients who may need palliative care. The program assesses patients and provides follow-up care, if appropriate. The pilot program saw an increase in the use of palliative care and hospice enrollment.
- Sutter Health-Palo Alto Medical Foundation offers LinkAges, a virtual bank of volunteer hours. The intent is for an able-bodied person to offer volunteer support to relieve family care giving responsibilities and help an elderly person stay in their home. The volunteer can cash in their hours for services, such as tutoring or home maintenance. This network seeks to address some of the isolation issues that many seniors face.
- The Southern California Permanente Medical Group (SCPMG) offers Complete Care: The program offer health education, outreach, physician education, pharmacy services, and case management to improve clinical outcomes and decrease costs.
- CalHR, SEIU Local 1000, State Treasurer’s Office, State Controller’s Office, CalPERS, and Kaiser Permanente offer Healthier U. The worksite wellness program aims to promote physical activity of state employees at work sites. The program includes online health competitions to eat healthier and exercise. There are also smaller scale interventions including healthy food potlucks and fitness/walk breaks organized by booster employees.
- The Partnership HealthPlan of California aims to reduce readmissions and transitions of care in the Medi-Cal program. The Care Transitions Pilot program uses an evidence-based model and assessment tool. In the first year, 13% of participants were readmitted in contrast to the expected average rate of 20% readmissions. The resulting savings yielded a return on investment of 2.7%. Due to increased savings seen in the first year of the pilot, the program was expanded from three to twelve sites.
For information, visit (https://innovationchallenge.forms.fm/lghc-innovation-challenge-2-0).
Millennial Women Face Financial Wellness Gender Gap
Even assuming that there is pay equity, Millennial women are falling short in retirement savings. Based on assumed contribution rates, younger men and women aren’t saving enough for retirement; the shortfall for a typical 25-year-old woman is 28% greater, according to a report by Financial Finesse. This difference is exacerbated when women take career breaks. Based on conservative estimates of wage inflation and time out of the workforce, an early career break can cost women $1.3 million in lost savings, with later career breaks costing less but still having sizable financial effects. As a result, Millennial women who take early career breaks will need to save 25% during their working years. More employers focusing on pay equity and flexible work environments to allow employees to better integrate work and life. Employers are increasingly offering financial mentorship programs to employees. For more information, visit https://ffinesse.box.com/v/2016GenderGap.
The Millennial Benefit Perspective Turning Stereotypes Around
Millennials have widely varying perspectives, life experiences, and attitudes toward their benefits, according to a MetLife study. The study looks at younger Millennials who are 21 to 24 and older Millennials who are 25 to 34.
Living Situations & Life Events
Forty-seven percent of younger Millennials, 70% of older Millennials, and 79% of Generation X live with a spouse or partner. The percentage of Millennials and Gen X-ers living with children under age 18 also increases at a similar rate. This sets up fundamental differences in lifestyles between the younger and older Millennials. Life events have a considerable effect on workplace benefit selections. Significant events include getting married, getting divorced, having children, changing employment, dealing with a death, or caring for an ailing parent. The triggers for benefit decision-making are quite different for younger and older Millennials. For example, 59% of younger Millennials and 73% of older Millennials say that these kinds of life events affect their benefit decisions. This suggests that older Millennials are making more family-focused benefit decisions as they are immersed in a life stage that’s full of changes.
Personalizing Benefits
Companies with more Millennials have made significant efforts to adapt their benefits. They are actively assessing and have even made changes to salaries (30% of companies with a low Millennial presence versus 42% of companies with a Millennial presence). Similar patterns surface when employers were asked whether they had increased benefits and bonuses. Moving benefit selections is becoming increasingly more common among employers with large Millennial populations. Employers with a high presence of Millennials are 10% more likely to offer benefits through an exchange compared to employers with a low presence of Millennials. Companies with higher populations of Millennials plan to move more employees to exchanges in the next two to three years. Helping younger Millennials understand and appreciate their benefits is as important as offering older Millennial benefits and tools they can use to adapt to their own life-changing events. A diversified approach will help ensure that all Millennials get the solutions they need.
Employers are taking notice that offering a wide array of customizable, non-medical benefits is important to Millennials, but there is room for improvement. Companies with a high Millennial count are much more willing to accommodate broader ranges of benefits compared to those with a low Millennial count. Companies with a medium mix of Millennials are most accommodating, with 60% willing to customize benefits to meet the needs of employees across all age groups. These companies with a medium mix also offer the most benefits and are more likely to provide elemental non-medical benefits, such as 401Ks, dental, life, prescription drug, and vision care coverage compared to employers with a low or high presence Millennials. Companies with a diverse spread of generations may be more likely to take the wants and needs of all generations into account, not only Millennials.
Fifty percent of companies with a high Millennial presence are likely to increase the number of non-medical benefits in the next few years, compared to 43% of companies with a medium Millennial presence, and 34% of companies with a low Millennial presence. The same holds true for wellness programs, automatic re-enrollment, and single carriers that offer multiple benefits. Employers with higher Millennial populations are more likely to offer these options and benefits that are of interest to Millennials. There is room for growth with additional benefit options. Fifty-four percent of older Millennials are interested in dependent coverage and automatic payroll deduction. They are also more interested in portable benefits than are younger Millennials. Yet, some employers are not yet offering these programs or benefits.
Prescription Drug Benefits
When it comes to must-have benefits, older Millennials and Gen X-ers have greater needs. For example, prescription benefits get more important as the age of the workforce increases. Forty-eight percent of younger Millennials consider prescription coverage to be a must-have benefit, compared to 64% of older Millennials and almost three-quarters of Gen X-ers. Older Millennials and Gen x-ers make up the majority of households with children, which further plays into how life stages and events drive benefit needs and considerations.
Financial Planning
Older Millennials are reviewing their retirement savings plans, re-balancing investment portfolios, and paying more attention to their benefit offerings. They also acknowledge that certain benefits can reduce their financial stress, such as short- and long-term disability. Most employers agree that they have a responsibility to help employees become more financially secure through benefits. Employers may benefit from greater Millennial loyalty if they broaden their attitudes and scope of responsibility.
Company Loyalty
The majority of Millennials are committed to their jobs. In fact, 64% of younger Millennials and 75% of older Millennials intend to be working for the same organization in 12 months. Fifty-nine percent of younger Millennials say they are committed to their organization’s goals, versus 72% of older Millennials. This percentage drops slightly for Gen X-ers. Over half of younger Millennials and 66% of older Millennials say that working for their employer motivates them to do the best work possible. It’s no surprise that financial concerns are heightened with the additional responsibility of a partner or a child. Older Millennials are most likely to be facing those responsibilities and suddenly have a myriad of concerns to consider. Is there enough money for their children’s college education? How are bills going to get paid if someone in the household loses their job or is no longer able to work? As Millennials face these questions, they have a renewed appreciation for their benefits. Fifty-seven percent of companies with a low Millennial presence consider loyalty an important factor in their benefit offering compared to 66% of companies with a medium Millennial presence, and 68% of companies with a high Millennial presence. Loyalty is also an important benefit strategy to employers with international employees. For more information, visit www.metlife.com.
California Health Care Foundation Offers Regional Market Reports
The California Health Care Foundation has published a series of reports highlighting trends in seven regional health care markets across California. The first focuses on how the Affordable Care Act (ACA) and market forces have spurred hospitals, physicians, and other providers to collaborate among themselves and with public and private payers to reform care delivery systems and payment methods. Most of these initiatives aim to slow the growth of health care spending and improve the coordination and quality of patient care. The second report focuses on collaborations and innovative approaches among California’s federally qualified health centers (FQHCs), other safety-net providers, and agencies. California’s FQHCs are key primary care providers for low-income people and have been expanding their capacity due to several market and policy factors, particularly the implementation of the ACA. To see the reports, visit http://www.chcf.org/almanac/regional-markets.
Consumers would benefit from reduced insurance licensing burdens
At the state and federal level, policymakers are examining ways to streamline and repeal burdensome occupational licensing laws. They should look at reforms to introduce more competition and choice to the market for insurance agents and brokers, according to a policy study from R Street Institute Senior Fellow R.J. Lehmann. As numerous studies have demonstrated, there is little evidence that a growing mountain of licensing red tape has protected the public. It has meant diminished opportunities for workers and entrepreneurs and mounting costs for consumers, Lehmann writes.
The national ubiquity of insurance licensing requirements makes complete abolition unrealistic. Moreover, independent insurance agents have been a powerful political force, and they have resisted change. But he also notes that agents have supported the creation of the National Association of Registered Agents and Brokers, which should streamline the process for interstate licensing.
Lehmann says that further reforms should include the following:
- Expand the ability of savings banks to sell life insurance without a producer’s license, as is permitted in New York, Connecticut, and Massachusetts.
- Create incentive programs to cut commissions in the federal crop insurance program,
- Create more limited line licenses for relatively vanilla insurance products, such as term life insurance.
- Abolish regulations in 48 states that bar agents and brokers from offering rebates to their customers.
Lehmann said “As consumers come to expect more choice in how they buy insurance, the market…will imagine new business models to provide that choice…Agents and brokers will have to adapt. To stay in the good graces of the public they serve, lawmakers and regulators will have to do the same.” For more information, visit www.rstreet.org.
Virtual Summit for Financial Advisors and Life Insurance Agents
The world’s first virtual summit for financial professionals, retirement planners, and life insurance advisors will be held online from November 11 to 17. For a limited time, free tickets are available at the summit website at www.VirtualAdvisorSummit.org.
Webinar: Post Pregnancy, Return to Work and the Law
What are employer obligations to employees after their pregnancies? What are best practices for those like intermittent bonding, post pregnancy restrictions, and state-specific nursing law? Find out at the next webinar hosted by the Disability Management Employer Coalition. It will be held Thursday, November 3 at 9:00 PST. To register, call 202-554-5796.
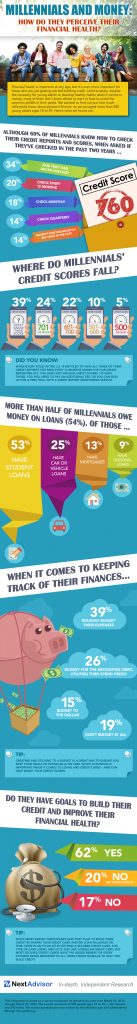
NextAdvisor Illustrates Millennials’ Financial Health